Congestive Heart Failure (CHF)
- General information: inability of the heart to pump an adequate supply of blood to meet the metabolic needs of the body.
- Types
- Left-sided heart failure
- Left ventricular damage causes blood to back up through the left atrium and into the pulmonary veins. Increased pressure causes transudation into the interstitial tissues of the lungs with resultant pulmonary congestion.
- Caused by left ventricular damage (usually due to an MI), hypertension, ischemic heart disease, aortic valve disease, mitral stenosis
- Assessment findings
- dyspnea, orthopnea, PND, tiredness, muscle weakness, cough
- tachycardia, PMI displaced laterally, possible S3, bronchial wheezing, rales or crackles, cyanosis, pallor
- decreased pO2, increased pCO2
- diagnostic tests
- chest x-ray: shows cardiac hypertrophy
- PAP and PCWP usually increased; however, this is dependent on the degree of heart failure
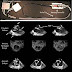
- Echocardiography: shows increased size of cardiac chambers
- Right-sided heart failure
- Weakened right ventricle is unable to pump blood into the pulmonary system; systemic venous congestion occurs as pressure builds up.
- Caused by left-sided heart failure, right ventricular infarction, atherosclerotic heart disease, COPD, pulmonic stenosis, pulmonary embolism.
- Assessment findings
- anorexia, nausea, weight gain
- dependent pitting edema, jugular venous distension, bounding pulses, hepatomegaly, cool extremities, oliguria
- elevated CVP, decreased pO2, increased ALT (SGPT)
- diagnostic tests
- chest x-ray: reveals cardiac hypertrophy
- echocardiography: indicates increased size of cardiac chambers
- High-output failure
- Cardiac output is adequate but exceeded by the metabolic needs of the tissues; the exorbitant demands made on the heart eventually cause ventricular failure.
- Caused by hyperthyroidism, anemia, AV fistula, pregnancy
- Medical management (all types)
- Determination and elimination/control of underlying cause
- Drug therapy: digitalis preparations, diuretics, vasodilators
- Sodium-restricted diet to decrease fluid retention
- If medical therapies unsuccessful, mechanical assist devices (intra-aortic balloon pump), cardiac transplantation, or mechanical hearts may be employed.
- Nursing interventions
- Monitor respiratory status and provide adequate ventilation (when CHF progresses to pulmonary edema).
- Administer oxygen therapy.
- Maintain client in semi- or high-Fowler's position.
- Monitor ABGs.
- Assess for breath sounds, noting any changes.
- Provide physical and emotional rest.
- Constantly assess level of anxiety.
- Maintain bed rest with limited activity.
- Maintain quiet, relaxed environment.
- Organize nursing care around rest periods.
- Increase cardiac output.
- Administer digitalis as ordered and monitor effects.
- Monitor ECG and hemodynamic monitoring.
- Administer vasodilators as ordered.
- Monitor vital signs.
- Reduce/eliminate edema.
- Administer diuretics as ordered.
- Daily weights.
- Maintain accurate I&O.
- Assess for peripheral edema.
- Measure abdominal girths daily.
- Monitor electrolyte levels.
- Monitor CVP and Swan-Ganz readings.
- Provide sodium-restricted diet as ordered.
- Provide meticulous skin care.
- Provide client teaching and discharge planning concerning
- Need to monitor self daily for signs and symptoms of CHF (pedal edema, weight gain of 1-2 kg in a 2-day period, dyspnea, loss of appetite, cough)
- Medication regimen including name, purpose, dosage, frequency, and side effects (digitalis, diuretics)
- Prescribed dietary plan (low sodium; small, frequent meals)
- Need to avoid fatigue and plan for rest periods.
Saturday, May 24, 2008
|
Labels:
cardiovascular disorder
|
This entry was posted on Saturday, May 24, 2008
and is filed under
cardiovascular disorder
.
You can follow any responses to this entry through
the RSS 2.0 feed.
You can leave a response,
or trackback from your own site.
Subscribe to:
Post Comments (Atom)






0 comments:
Post a Comment